REGISTER NOW!
Register online: thefpm.org.uk/fpm-at-100
Email leastman@bmj.com for further details
Registration: Standard £75 (£50 for trainees) PMJ or HPT authors £50 (£30 for trainees)
Approved (code 121386) by the Federation of the Royal Colleges of Physicians of the United Kingdom for 6 category 1 (external) CPD credits.
Poster abstracts
1. Medicine use and medicine-related problems in patients with liver cirrhosis: a systematic review of quantitative and qualitative studies.
Ejaz Cheema1, Abdullah Al-Hamid1, Aliaa Al-Aryan2
1University of Birmingham, 2University of Hertfordshire
Introduction: Liver cirrhosis is a major chronic disease that is associated with high morbidity and mortality [1]. The associated co-morbidities and medical complications together with the use of complex and multiple drug therapies by patients with liver cirrhosis put them at an increased risk of developing medicine related problems (MRPs). MRPs can be defined as an event or circumstance involving drug therapy that actually or potentially interferes with desired health outcomes [2]. This review aims to systematically investigate the prevalence, causes and risk factors of MRPs in cirrhotic patients and to explore factors influencing the medicine use from patients and health care providers’ perspectives.
Subjects and Methods: Eight online databases (PubMed, Scopus, CINAHL, The British library, PsycINFO, Web of Science, EMBASE, and Google scholar) were searched up to 30th Sep, 2018 with no start date. Both quantitative studies including randomised controlled trials (RCTs), clinical trials and observational studies as well as qualitative studies were included in the review. Search terms used included ‘medicine related problems’, ‘medicine use’, ‘patients’ perceptions’ and ‘adverse drug reaction’. Data collected included the study design, baseline characteristics of study population and study outcomes. Appropriate Critical Appraisal Skills Programme (CASP) tools were used to assess both the quality of quantitative studies and qualitative studies. An in-depth descriptive analysis of the quantitative data and a thematic analysis of the qualitative data were undertaken.
Results: 16 quantitative studies and 11 qualitative studies were included in the review. Of the 16 quantitative studies, nine examined the prevalence, causes, risk factors and medicine classes associated with MRPs and the remaining seven studies reported factors affecting medicine use. Mean frequency of MRPs reported in the quantitative studies ranged from 14-23.4%. The most frequent causes of MRPs identified in the studies included drug interactions, inappropriate dosing and use of contraindicated drugs. Major risk factors associated with MRPs included polypharmacy, severity of liver disease and length of hospital stay. Diuretics, analgesics and sedatives were suspected to be among the most common drug classes associated with MRPs. The thematic synthesis of qualitative data identified three key themes: patient related factors including lack of patients’ knowledge about liver cirrhosis and its risk factors; health care related factors including lack of communication between healthcare professionals and patients; stigma and negativity including negative attitudes (misconceptions and discriminations) and negative consequences of liver cirrhosis.
Conclusions: MRPs pose a significant social and financial burden on both patients and healthcare systems. Findings of this review suggest that the management of liver cirrhosis should not only be limited to the provision of safe and effective drug therapy but should also expand to improving the understanding and awareness of patients about the disease. Future research should focus on assessing the impact of patient-specific education on medicine use by patients with liver cirrhosis.
1. Murray CJ, Vos T, Lozano R, et al. Disability-adjusted life years (DALYs) for 291 diseases and injuries in 21 regions, 1990-2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet. 2012, 380: 2197-2223.
2. Strand L, Morley P, Cipolle R, Ramsey R, Lamsam G. Drug‐related problems: their structure and function. DICP 1990; 24: 1093–1097.
2. Pompholyx – a rare side effect of trastuzumab.
Abubakkar Raheel, Syed Irfan Wafa, Anupama Gore
University Hospitals of Leicester, Leicester Royal Infirmary
Background Trastuzumab is a monoclonal antibody prescribed as part of systemic treatment of breast cancer. Trastuzumab can be prescribed on its own or as an adjuvant with chemotherapy or hormone therapy against over-expressing HER2 positive breast cancer. Patients on Trastuzumab can develop side effects of nausea, vomiting, cardiotoxicity and flu-like symptoms [1] . However, we describe a rare side effect of Pompholyx (dyshidrotic eczema). This may be the first case of this presentation to be reported.
Case presentation A 50-year-old Caucasian female with a background of 3mm invasive ductal carcinoma of left breast presented with extensive vesicles and blistering on palms of hands and feet following treatment with trastuzumab [Figure. She had wide local excision of a 3mm invasive ductal carcinoma of left breast in January 2018 and sentinel lymph node biopsy which revealed a grade 2, HER2 positive, node negative, breast cancer. She received 6 cycles of adjuvant chemotherapy with epirubicin and cyclophosphamide followed by 15 fractions of 40 Gy adjuvant radiotherapy. Thereafter she was commenced on targeted therapy with trastuzumab. After the 2nd cycle of trastuzumab she developed multiple small vesicular eruptions predominantly on the hands and feet, which worsened by the 3rd cycle. These were diagnosed by a dermatologist as extensive pompholyx, which was treated with topical steroid, emollient, potassium permanganate and fludroxycortide tape on the palms. Her swab cultures grew Staphylococcus aureus and beta-hemolytic streptococcus group-A, which was subsequently treated with intravenous flucloxacillin with a modest response.
Discussion Trastuzumab is a humanized monoclonal antibody that blocks HER2 receptors, undermining HER2 signaling in HER2 over-expressing breast cancers. The pathogenesis of pompholyx [2] is not well understood thus it is difficult to establish a direct connection with trastuzumab at this stage. According to some immuno-histo chemistry studies, strong presence of CD3, CD8, CD45 as well as anti-human antibodies are found in pompholyx whereas an immune mediated T-Cell lymphocyte-driven response in suppressing tumor growth in cancer has extensively been described. We plan to biopsy the lesions and subsequently monitor her response to steroids with continuation of trastuzumab, since benefits of trastuzumab outweigh the risks of eczema [3].
Figure. Multiple cutaneous lesions on the palm, finger and toe. Images consented for teaching in the healthcare context. © University Hospitals of Leicester NHS Trust (Dept of Medical Illustration).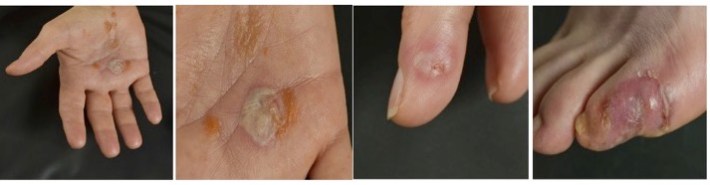 Conclusions We report the first case of trastuzumab therapy presenting with extensive infected pompholyx (dyshidrotic) eczema in a breast cancer patient. Although the patient described a history of a mild eczema five years previously, an acute flare while undergoing treatment could certainly be added to conditions at risk of flare during trastuzumab therapy until this is proven as a clear trastuzumab side effect through meta-analysis of multiple studies and a comprehensive dataset.
Conclusions We report the first case of trastuzumab therapy presenting with extensive infected pompholyx (dyshidrotic) eczema in a breast cancer patient. Although the patient described a history of a mild eczema five years previously, an acute flare while undergoing treatment could certainly be added to conditions at risk of flare during trastuzumab therapy until this is proven as a clear trastuzumab side effect through meta-analysis of multiple studies and a comprehensive dataset.
1. Baselga J , Cortés J , Kim SB , et al; CLEOPATRA Study Group. Pertuzumab plus trastuzumab plus docetaxel for metastatic breast cancer. N Engl J Med. 2012;366:109–19. doi:10.1056/NEJMoa1113216
2. Ana Maria Abreu-Velez, Frank J. Pinto, Jr, Michael S. Howard. Dyshidrotic eczema: relevance to the immune response in situ. N Am J Med Sci. 2009;1: 117–120. PMCID: PMC3364640
3. Chang HR . Trastuzumab-based neoadjuvant therapy in patients with HER2-positive breast cancer. Cancer. 2010;116:2856–67.doi:10.1002/cncr.25120
3. Evaluation of HO-1 involvement in melanoma resistance to BRAF inhibitor vemurafenib.
Giulia Loi, AnnaLisa Furfaro, Maria Adelaide Pronzato, Gabriella Pietra, Mariapaola Nitti.
Department of Experimental Medicine, Section of General Pathology,
University of Genoa, Via Leon Battista Alberti, 2 16132 Genova (GE), Italy.
Introduction The point mutation of the BRAF gene (BRAFV600E) is present in more than 50% of melanoma. This mutation determinate the continuous activation of MAPK pathway, which favours cell survival and proliferation. Vemurafenib/PLX4032 (PLX4032) is an inhibitor of BRAFV600 used for the therapy of these tumours, but, after an initial positive response, in many cases a relapse of the disease occurs. HO-1 is the inducible form of heme oxygenase and overexpression is involved in the growth and resistance to therapy of different types of tumours. In this study we have evaluated the involvement of HO-1 in chemoresistance and angiogenesis of BRAFV600E primary melanoma cells.
Materials and Methods We used a primary melanoma cell line, derived from a metastasis from a patient, and exposed cells to PLX4032 (1-10μM). The role of HO-1 was studied by gene silencing or using the pharmacological inhibitor of HO-1 tin-mesoporphyrin IX (SnMP-IX), a drug used to treat hyperbilirubinemia. Angiogenic potential was evaluated by using bovine aortic endothelial cells (BAEC) isolated in our laboratory.
Results Primary melanoma cells (MeOV-1) were exposed to 1-10μM PLX4032 for 24h. MTT and Trypan blue assays showed a reduction in cell viability of 45% and immunoblot and qRTPCR analyses revealed a significant upregulation of HO-1 expression. HO-1 silencing or exposure to 10μM SnMP-IX further decreased cell viability after exposure to PLX4032. Subsequently, we evaluated the angiogenetic potential of melanoma cells. Medium derived from MeOV-1 cells, exposed to 10 microlar PLX4032, was used to treat BAEC seeded on Matrigel. Tube formation, branching and density were increased in comparison to BAEC exposed to the medium from untreated MeOV-1 cells. Interestingly, when BAEC were treated with conditioned medium from MeOV-1 cells and HO-1 was silenced, 10μM PLX4032 showed a reduced ability to form tubes.
Conclusions These results highlight an important role of HO-1 in favouring melanoma resistance to target therapy and angiogenesis.
Supported by the University of Genoa, Department of Experimental Medicine.
4. Which intensive care analytics are a worthwhile investment for developers? An early health technology assessment.
Lytske Bakker, Jos Aarts, Ken Redekop.
Erasmus School of Health Policy and Management, Erasmus University
Introduction In intensive care (IC), monitoring data are continuously being collected. Unfortunately, this data is often not interpretable for clinicians and therefore goes unused. While advanced analytics can process this data to support improvements in patient care, developers ideally invest in those analytics that lead to the greatest health benefits or cost reductions. We explored the potential cost-effectiveness of three IC analytics.
Subjects and Methods We assessed the cost-effectiveness of three applications: the early identification of catheter-related bloodstream infection (CRBSI), improved nutrition monitoring and identification of high driving pressure (HDP) in ventilated patients. The literature was used to populate the decision trees and patient data from a Greek IC were used for the nutrition and HDP estimates. We performed univariate, multivariate, and probabilistic sensitivity analyses.
Results Early identification of CRBSI reduced mortality and length of stay, thereby increasing quality-adjusted life-years (QALYs) (6.70 vs. 6.58) and reducing costs (€8,183 vs. €9,869); probability of CRBSI and the costs per IC day were key influencers of the ICER and the probability of dominance was 90%. Improved nutrition monitoring could increase nutrition adherence (0.37% vs. 0.03%) and decrease costs by reducing length of stay (€9,988 vs. €10,720). For HDP, benefits were limited, resulting in higher costs as well as minimal and highly uncertain health benefits.
Conclusions Developers should study the potential impact of the analytics they wish to develop before investing time and money. We illustrate that analytics for early identification of CRBSI and improved nutrition monitoring are worth further investment while identifying HDP may not be. The other factors that influence success besides health and financial benefits such as the competition and data access should be assessed.
This research was part of the European AEGLE project and received funding from the European Union’s Horizon 2020 Research and Innovation Programme under grant agreement No. 644906.
5. Investigating the effect of catecholamines on ischaemia-induced ventricular fibrillation when in the presence of an intraventricular balloon.
William Pickles, Michael Curtis
King’s College London, UK
Introduction Sudden cardiac death (SCD) is the greatest cause of cardiovascular disease-related mortality. Lethal ventricular fibrillation (VF), arising from myocardial infarctions is the most prominent cause of SCD. The isolated rat heart is widely used to model ischaemia-induced VF owing to its ability to produce high baseline incidences of VF and the ability to regulate several known arrhythmogenic mediators. A model that allows concurrent assessment of VF and contractile function would halve animal requirements. Unfortunately, in Langendorff perfused rat hearts, IVB inflation inhibits the ability of regional ischaemia to elicit VF (1). However, perfusion with catecholamines facilitates ischaemia-induced VF (I-IVF) in IVB-free hearts when risk of VF is low due to a small ischaemic territory (2). Therefore, it was sought to overcome the IVB-induced VF suppression by perfusion with exogenous catecholamines: rendering a model in which the antiarrhythmic properties and the effects on heart dynamics a potential drug has could be assessed simultaneously. Here we tested whether catecholamines can surmount the antiarrhythmic effect of IVB inflation.
Methods Male Wistar rat (285-400g) hearts were Langendorff-perfused with an IVB positioned in the left ventricle and minimally inflated (0.01 ml) to give a detectable developed pressure (~30 mmHg; ‘IVB’ groups) or inflated substantially (0.12 ml) to give a developed pressure >100 mmHg (‘IVB inflated’). Baseline assessment (-11 min) during perfusion with Krebs’ (modified to contain 4mM K+) was followed by randomized and blinded switch to test solution at -10 min, then left coronary artery ligation at time zero, with ischaemia maintained for 60 min. Test solution comprised Krebs’ containing catecholamines (93.9 nM noradrenaline and 22.5 nM adrenaline in 15 mM ascorbate vehicle) or vehicle alone (n = 9/group). Design (blinded and randomized) and data analysis (e.g. use of ANOVA for Gaussian-distributed data and Fisher’s exact test for VF incidence) accorded with BPS guidelines (3).
Results Heart rate and developed pressure were increased by catecholamines (Cat) from 1 min before ligation (-1 min) (294±6, 310±13 to 437±10, 442±13Beats/min and 28±2, 101±3 to 94±14, 177±10mmHg for IVB and IVB inflated groups respectively), and the effect on pressure was exacerbated by IVB inflation (IVB 30±3mmHg vs IVB inflation 101±3mmHg). Ischaemia reduced developed pressure, with effects sustained during ischaemia. Mean ischaemic zone size varied between groups from 53±2 to 59±1% (P>0.05). Cats increased VF incidence (Vehicle 0% vs Cats 56%) (P<0.05) and extended the susceptibility time window past 30 min of ischaemia, but IVB inflation was antiarrhythmic during ischaemia and surmounted the arrhythmia facilitating effect of catecholamines (IVB inflated+CATs 0% vs IVB+Cats 56%).
Conclusions Catecholamine perfusion was unable to surmount IVB-induced VF suppression. Unfortunately this rendered VF incidence too low to permit the assay to be suitable for evaluating drug effects on VF and contractile function contiguously.
1. Wilder CDE, et al., (2016). Br J Pharmacol 173, 39-52
2. Wilder CDE et al., (2016). http://www.pa2online.org/abstracts/vol13issue3abst245p.pdf
3. Curtis MJ, et al., (2015). Br J Pharmacol 172:2671-2674, 2015
6. Zinc attenuates UVA-dependent labile iron increase in human dermal fibroblasts: implications for skin ageing.
Matthew Smith, Adomas Rimdeika, Richard Siow, Richard Naftalin.
King’s College London, UK
Introduction To protect the cell from damaging oxidative stress induced by Fenton reactions, the cytosolic labile iron pool (LIP) is normally kept low and tightly regulated. These reactions are initiated by interactions between iron and hydrogen peroxide and can be prolonged and increased with ascorbate. The source of cytosolic labile iron is unclear. It has been suggested that lysosomes are the main source of iron, since protease inhibitors reduce leakage of lysosomal contents including iron after UVA (ultraviolet light) exposure. However, the time resolution of the changes in enzyme activity required to assess lysosomal leakage is too long to establish whether lysosomal damage occurs due to secondary response to iron release from other sources, particularly ferritin. Other methods are therefore required to clarify the source of cytosolic labile iron. Zinc is a redox-inert metal that has anti-oxidant, anti-inflammatory and anti-proliferative properties which is notably reduced in patients with subclinical carotid atherosclerosis, acute coronary syndrome and heart failure. Zinc is known to block iron diffusion via ferritin threefold channels and can therefore be used as a tool to examine UV-induced iron release from ferritin.
Methods A fluorescence probe (FeRhoNox-1) specific for ferrous ion was used to determine the time dependent changes in human fibroblasts following exposure to UVA irradiation. Since it is known that low concentrations of zinc block iron diffusion via ferritin threefold channels, we reasoned that pre-incubating skin cells with low concentrations of ZnCl2 would inhibit iron release from ferritin after photo-activation by UVA. Confluent monolayers of human dermal fibroblasts were incubated overnight with 10mM FeSO4 and 0, 10 and 40mM ZnCl2, before being loaded with FeRhoNox-1 and exposed to UVA (360nm) for 1-10min (8 – 80 J/m2), with fluorescent readings gathered at 1 minute intervals.
Results The control cell iron dependent fluorescent signal increased by approximately 100% after 10 min UVA irradiation compared to pre-UV baseline (P < 0.001). This UVA-dependent increase in cell iron is prevented by both 10 and 40 mM ZnCl2.
Conclusions These results suggest that UVA causes a significant increase in skin fibroblast LIP and hence oxidative stress which may exacerbate the ageing phenotype of dermal cells. This LIP is likely to be sourced mainly from ferritin since this is completely blocked by relatively low concentrations of extracellular ZnSO4.
7. Dietary sulforaphane reduces peri-infarct constriction frequency in mouse brain following focal cerebral ischaemia via a Nrf2-independent mechanism.
Keith Farrell-Dillon, Paul A. Fraser, Giovanni E. Mann
BHF Centre of Research Excellence, School of Cardiovascular Medicine & Sciences, King’s College London, UK
Introduction The dietary isothiocyanate sulforaphane (SFN) obtained from precursors in cruciferous vegetables such as broccoli is a potent inducer of endogenous antioxidant defences. As a strong electrophile, it oxidises cysteine residues in the redox sensor Keap1 inducing activity of the transcription factor Nrf2 and upregulation of target antioxidant and detoxifying genes. We have previously demonstrated that oral administration of doses achievable through diet for three days prior to surgically induced ischaemic stroke results in a reduced infarct volume 70 h later in wild type but not Nrf2 deficient mice, possibly as a consequence of enhanced Nrf2-mediated redox protection in the context of ischaemic-reperfusion injury.
Materials and Methods To further investigate mechanisms by which dietary sulforaphane affords neuroprotection, we measured acute blood flow changes during and after focal cerebral ischaemia in mice fed vehicle (corn oil) or sulforaphane at 5 mg/kg for 3 days. Ischaemic stroke was induced via the Longa procedure, employing a surgically inserted filament to transiently occlude the middle cerebral artery under stereotaxic anaesthesia. Ischaemia followed by 60 min of reperfusion resulted in a reproducible temporal lobe stroke. Transcranial laser speckle imaging (Moor FLIPI 2) was used to assess blood flow with high temporal (20 s) and spatial (20 μm) resolution, enabling discrimination of three functional regions during stroke in the unaffected contralateral hemisphere, partially responsive per-infarct region and the ischaemic infarct core.
Results While sulforaphane did not alter initial baseline blood flow or affect the depth of ischaemia at the start of the procedure, a clear effect was resolved on the number of evoked peri infarct constriction (PIC) waves. While in both vehicle and treatment groups, an initial PIC was observed in all animals within 10 minutes of the onset of ischaemia, sulforaphane pre-treatment in wild type mice significantly reduced the number of subsequent PICs. In Nrf2 deficient mice, an equivalent and statistically significant reduction in PIC number was seen associated with sulforaphane pre-treatment, implying that the effects of sulforaphane on PIC frequency are unlikely to be mediated by Nrf2 but rather associated with associated redox gene induction. As sulforaphane significantly improved post-reperfusion core blood flow in wild type not Nrf2 deficient mice.
Conclusions Our findings suggest that peri-infarct depolarisation waves or baseline Nrf2 genetic status are not major contributors to post-reperfusion, no-reflow in ischaemic stroke. However, activation of Nrf2 target genes by dietary sulforaphane protects against no-reflow pathology with persistent benefits post stroke.
Supported by the British Heart Foundation
8. Defining the normal spectrum of electrocardiographic and structural adaptations of white, black and mixed-race adolescent athletes’ heart.
Aneil Malhotra, Sanjay Sharma
St. George’s University of London and Hospital
Introduction This study aimed to describe the normal spectrum of EKG changes and left ventricular dimensions in a large cohort of healthy white, black and mixed-race, male and female adolescent soccer players. There are a paucity of data describing the adolescent athlete’s heart with the vast majority of studies based on adult white athletes. Not only are adolescent athletes (aged 14-18 years old) significantly understudied compared with adults but are more vulnerable to sudden cardiac death than adults. There is a four to six-fold higher incidence of sudden cardiac death (SCD) during exercise among young black athletes (aged 14-35 years) compared with young white athletes. Such a significant disparity has never before been systematically explored, due to the limitations in identifying individuals at risk and a consequent lack of a well-defined population. The population of black individuals in the UK is 8 million, making up 13% of the overall population. In professional sport however, black athletes constitute up to 30% of all sportsmen and sportswomen. Moreover, the mixed-race athlete’s EKG and echocardiogram has not before been described, though this is the fastest growing ethnic group participating in sport in the UK and US and for whom no such previous data exist.
Methods Between 1996 and 2016, 11,435 consecutive adolescent soccer players underwent pre-participation screening. 11,168 soccer players (mean age 16.4±1.3 years) were evaluated with an EKG and echocardiogram measuring maximal left ventricular wall thickness (MLVWT) and left ventricular end diastolic diameter (LVEDD). Ethnicity was self-reported in accordance with UK census classification.
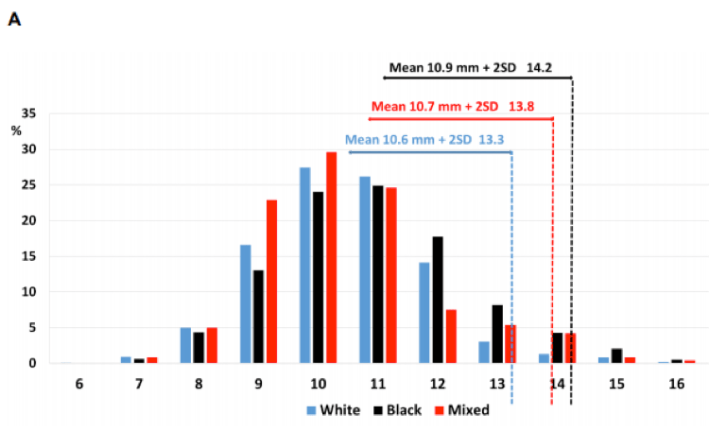
Results The cohort included 10,581 (95%) males and 587 (5%) females. There were 9,664 (87%) white, 1,004 (9%) black and 500 (4%) mixed-race athletes. Black male athletes exhibited a greater MLVWT compared with both white (10.9 vs. 10.6mm; p=0.0323). (Figure 1A). White male athletes demonstrated the largest LV cavity sizes compared with black athletes (52.4 vs. 50.6mm; p=0.0477). Black female athletes revealed a greater MLVWT compared with white female athletes (8.6 vs. 8.2mm; p=0.0352; (Figure 1B). As with males, white female athletes demonstrated larger LV cavity sizes than black athletes (46.3 vs. 45.2mm; p=0.0088) and mixed-race athletes (46.3 vs. 45.4mm; p=0.0316).
For white males, a proposed upper limit for MLVWT is 13mm and for black and mixed-race males <14mm. For females of all three ethnic groups this cut off is <11mm. Proposed upper limits for maximal LVEDD for white male is <60mm and for black and mixed-race males <59mm. For all females the cut-off is <52mm.
Conclusions Black athletes of both sexes reveal the greatest wall thickness compared with mixedrace and white athletes. Conversely, white athletes display the largest cavity size in both sexes. Mixed-race athletes demonstrate electrocardiogram and echocardiogram features more similar to black athletes than white athletes. Information regarding the upper limits of normality in this age group is useful in enabling the differentiation between physiological adaptation and cardiomyopathy.
Figure 1: Bar chart demonstrating the distribution of maximal left ventricular wall thickness in adolescent (A, top) male and (B, bottom) female athletes of white, black and mixed-race ethnicity. Upper limits according to 2 standard deviations (SD) are also shown.

9. p62 deficiency protects against cerebral ischaemia in insulin resistant mice.
Siddall, Keith Farrell-Dillon, Paul Fraser, Giovanni Mann, Sarah Chapple
King’s College London, UK
Introduction & aim Diabetic patients have poorer outcomes following ischaemic stroke. In rodents, similar findings are reported, with Type 1 and 2 diabetic rodents demonstrating increased infarct volume and worsened post-stroke recovery, which correlate with markers of autophagy overactivation post-ischaemia. p62 is a selective adaptor protein for autophagy, with mice lacking p62 (p62 KO) known to develop obesity-linked insulin resistance in adulthood and have supressed autophagic flux. To ascertain whether p62 is associated with ischaemic stroke pathophysiology, we evaluated post-stroke infarct volume and functional recovery in wild type (WT) vs p62 KO mice.
Methods All procedures were performed in male 8-9 week old C57BL/6 mice in accordance with the ARRIVE guidelines and Home Office regulatory approval. Transient focal ischaemia was induced by middle cerebral artery occlusion (MCAo) for 1h followed by reperfusion for 72h. Adhesive removal and open field assays were conducted daily 3 days prior to and 72h post-stroke to assess sensorimotor and motor function. Mice were then euthanised and brains perfused-fixed to obtain 10µm sections every 1mm relative to bregma. Infarct volume and astrocytosis were quantified using nissl staining and GFAP immunofluorescence, respectively. Data were analysed by unpaired student’s t-test or 2-way ANOVA and Bonferroni post-hoc test as appropriate.
Results Infarct volume assessed by nissl staining showed a significant (p<0.01) reduction in p62 KO vs WT mice (16±3 vs. 30±1 % brain volume, respectively). Proliferation and activation of astrocytes assessed by GFAP staining was found to be reduced in the peri-infarct border in p62 KO vs WT mice (p<0.05). Furthermore, p62 KO showed marked improvements in post-reperfusion functional recovery. Reduced motor function was observed in WT mice, with a ~70% reduction in max speed and total displacement vs baseline observed 72h post-reperfusion (p<0.01). No such impairments were reported in p62 KO mice. Similarly, sensorimotor function was impaired in WT mice post-reperfusion, with an increase in adhesive removal time in the affected (227±32 vs 29±9ms at baseline, p<0.001) and unaffected (73±23 vs 16±3ms at baseline, p<0.05) paw. p62 KO mice were protected, with adhesive removal times in the affected (51±44 vs 28±7ms at baseline, p<0.05) and unaffected (61±39 vs baseline 28±7ms at baseline) paws substantially improved when compared to WT mice at 72h.
Conclusions Our findings show that p62 KO mice are protected from cerebral ischaemia. This protection persists despite p62 KO mice being glucose intolerant, suggesting that p62 may be a meaningful therapeutic target even in comorbid diabetic populations. Further studies are needed to ascertain whether short-term functional recovery afforded by p62 deficiency persists long-term.
10. Evidence that altered redox status results in KCa3.1 channel reduced endothelial cell surface expression.
Paul Fraser1, Anas Bani Khalaf1, Giovanni Mann1, Matthew Smith1, Geraldine Clough2
1King’s College London, 2University of Southampton, UK.
Introduction Endothelial derived hyperpolarization (EDH) is an important path to vasodilatation especially in small arteries, and is more important in women and the elderly. Our previous work has shown that this becomes impaired in mice that had experienced a high fat diet during gestation up to weaning, with concomitant reduction in endothelial surface KCa3.1 expression [1]. We have tested the idea that altered redox status affects the location of KCa3.1 in human dermal microvascular endothelial cells (HDMECs).
Methods HDMECs were obtained from PromoCell (Heidelberg, Germany) and cultured in MV2 growth medium containing 1% penicillin-streptomycin in 5% O2, 5% CO2 at 37⁰C to passage 6 & 7 in the SCI-tive Physiological Oxygen Workstation from Baker Ruskinn (Maine, USA) for at least 5 days before experiments. The cells were plated on fibronectin (10 µg.ml-1) coated 8 well micro-slides (Ibidi, Martinsried, Germany) and incubated for 48h, treated with PBS or H2O2 100µM in PBS for 10min., and fixed with 4% formalin. Immunofluorescence was performed by incubating with anti-KCa3.1 mouse monoclonal antibody (AL-051 Alomone, Israel) at 4⁰C overnight, with half of the wells being treated with 2% Triton-X to permeablize the cells. The Alexa 488 labelled anti-mouse antibody for 1h and Texas Red Lycopersicon Esculentum Lectin (to stain the cell surface) for 20 min, were applied to the cells at room temperature and finally the DAPI nuclear stain was applied for 3 min. The cells were examined using a x60 1.3 NA oil-immersion objective and images captured via a Hamamatsu RG3 camera into a computer. Using ImageHopper software and computer-driven focussing device (Prior Instruments, UK) we took 10 serial images of KCa3.1at 1.0 µm intervals, which were integrated using Image J. These images were analysed for the fractional area of an endothelial cell occupied by KCa3.1, defined as bright spots between 1 to 4 µm diameter in the relevant fluorescence channel.
Results The density of channels on the surface, defined as the integrated image of non-permeablized KCa3.1 channels, was 9.5 ± 0.68 µm-2x103 (mean ± sem) , while in the permeablized cells the density within the whole cell area was 13.9 ± 1.89 µm-2x103 (p<0.05, ‘t’ test, 4 experiments with 20 cells per experimental group) indicating that about 70% of the channels normally reside on the cell surface. Treatment with H2O2 had little effect on the total cell density (reduced to 12.3 ± 1.56), but reduced the surface density to 5.25 ± 0.47 (p<0.01) i.e. reduced to 43%.
Conclusions Thus even a brief exposure to oxygen stress will result in the diminution of KCa3.1 on endothelial surface, and this may have implications for the ability of arterioles to dilate.
1. Stead R et al. (2016) J Hypertens. 34:452-63
11. Uptick/downtick – The future of morbidity and mortality meetings.
Helen Walker1, Steve Harris1, Aasiyah Rashan2
1University College Hospital, 2INFORM project
Introduction Morbidity and mortality (M&M) meetings are a national requirement for all departments in hospital. While they should confer improvement in education and patient care, they often ‘lack defined structure, resource support and…heterogeneity in case evaluation’ [1]. UK critical care has an embedded routine audit data collection on outcomes which is exported to a central body, Intensive Care National Audit & Research Centre (ICNARC), for cleaning and analysis. This data is submitted monthly but is returned on a quarterly basis preventing the timely identification of deaths or survivals that are unexpected (based on case-mix). In critical care, where the expected mortality is high, attention is fatigued if all mortality is reviewed and a more specific approach is required. A fundamental prerequisite for a good M&M meeting is appropriate, targeted case selection. Currently, time is wasted reviewing cases that are selected without systematic focus on ‘important variation’, so contemporaneous feedback on care is lost and learning and engagement are diminished. To combat this, we have developed a timely, targeted and transformative M&M based on data-driven case selection.
Methods We used code in R to generate an automated variable life-adjusted display (VLAD) chart using near real-time routine data from electronic health records. This reveals high yield outlying ‘uptick/downtick’ patients (patients who survived and should have died and vice-versa; Figure). We Identified crucial learning points from the clinical documentation of those selected ‘uptick/downtick’ patients using a specially developed Intensive Care Unit Structured Case Note Judgement Review format. We presented these targeted cases in a structured multi-disciplinary setting to key personnel to highlight the impact of timely narrative feedback, promoting staff engagement and morale and encouraging the growth of a proactive culture of safety and quality.
Results The VLAD cumulatively charts the effect of each individual admission using the ICNARC generated probability of death. Each death represents a ‘downtick’ in the plot and each survivor represents an ‘uptick’. When a patient predicted to survive dies, then the downtick will be prominent (conversely a patient who survives despite a high predicted mortality will make a prominent uptick).
Figure. A VLAD to show haematology and non-haematology mortality on ICU.

Conclusion Our M&M model is an original in-depth and specific data mine of critical care patient morbidity and mortality. This unique process seeks to provides an enabled and focussed method of case selection and emphasise the potential marginal gains that can be made in patient care. Over time, it will improve future clinical decision making and therefore patient outcomes.
1. Vreugdenburg et al., Morbidity and mortality meetings: gold, silver or bronze? ANZ Journal of Surgery. 2018;88:966-974.
12. Potential cost-effectiveness of spectral photon-counting computed tomography (SPCCT) versus CT combined with CT angiography (CTA) in the identification and treatment of ischaemic stroke patients in the UK
Anne Claire Peultier, Ken Redekop, Hans Severens
ESHPM Erasmus University, Rotterdam, The Netherlands
Introduction In current care, eligibility for thrombolysis or mechanical thrombectomy as acute stroke treatments is based on imaging (CT and CTA), time since onset and patient history. Thrombectomy will be routinely commissioned by NHS England provided it can be achieved within 6 hours of the onset of stroke. In case advanced imaging indicates salvageable brain tissue beyond the 6-hour window, thrombectomy will be commissioned up to 12 hours after stroke onset. SPCCT is an emerging technology expected to have an increased resolution. Besides identifying ischaemic stroke patients, SPCCT is expected to provide information about the presence of salvageable brain tissue and, in turn, identify those who are likely to benefit from thrombectomy beyond 6 hours. The aim of this study was to investigate the potential cost-effectiveness of SPCCT (versus CT+CTA) in identifying and treating ischaemic stroke patients in the UK.
Methods A decision-analytic model built on a decision tree and a Markov trace was developed. A hypothetical cohort of suspected stroke patients aged 74 was modeled (first stroke ever). Costs, outcomes and probabilities were obtained from the literature. Outcomes of the model included costs, life-years, quality-adjusted life-years, and incremental cost-effectiveness ratios. Univariate and probabilistic sensitivity analyses were performed.
Results Three scenarios were simulated in which the proportion of patients referred to thrombectomy after 6 hours was varied from 5%, to 10% and to 15% with SPCCT while it remained constant to 0% with CT-CTA. Three levels of SPCCT accuracy were simulated (perfect positive predictive value (PPV) (100%), intermediate PPV (78.1%), and low PPV (46.9%)). Over the three-month and lifetime horizons, all SPCCT-based scenarios improved QALYs and LYs compared to CT-CTA. Based on the currently used estimates, the probability that SPCCT is cost-effective at a willingness-to-pay threshold of £10000 per QALY is above 50% in all scenarios.
Conclusions Based on preliminary results, replacing CT-CTA with SPCCT to identify and treat ischaemic stroke patients beyond 6 hours may be good value for money. However, additional data regarding clinical outcomes following SPCCT based strategies are needed before the cost-effectiveness can be fully assessed.
|
13. Audit of a newly developed ambulatory care service at Diana Princess of Wales Hospital Grimsby UK.
Asem Ali, Jaidev Karmani
Northern Lincolnshire and Goole NHS Foundation Trust, UK
Introduction The aim of the ambulatory care unit to enable patients to be assessed, observed, diagnosed and treated without the need to be admitted to hospital and meeting their clinical needs by greater consistency of care through reduced clinical variability and improved patient experience, which can potentially reduce the number of clinical admissions, reduce time spent in hospital and helping to reduce overcrowding in the Emergency Department. We looked at performance of newly developed ambulatory care service at Diana Princess of Wales Hospital over 30 days period.
Methods Ambulatory care patients were selected who attended the service from 1st of October 2017 to 30th of October 2017. Information was collected by looking at the ambulatory care record spreadsheet, medical notes, discharge letters and hospital ambulatory care data. Service impact was analysed by numbers of service consumers, source of referral, impact on Accident and Emergency four hours target, appropriateness of referral, zero day discharges, length of stay for inpatients and diagnosis at discharge.
Results Patients were admitted to ambulatory care using the AMBS criteria and different ambulatory care models. Over the 30 day period, 260 attendances were recorded (male 123, female 137) which was 20% of the total medical admissions. 8 % of the referrals were from the Accident and Emergency Department. The majority of patient were referred as chest pain and shortness of breath, the most common diagnosis being musculoskeletal chest pain. Other diagnoses included cellulitis, pulmonary embolism, respiratory tract infection, angina and urinary tract infection. More than 92% of the patients were discharged same day. Only 8% of the patients were admitted to the Acute Admission Unit and among these 50% of the patients were referred inappropriately. 16% of patients were classed as re-attendees, mainly for treatment with iv antibiotics for cellulitis or pending next day investigation. The percentage of zero day discharges increased to 15% and there was an improvement in the Accident and Emergency four hour target exceeded to 5%.
Conclusion The newly developed ambulatory care service has helped to increase zero day discharges and improved the Accident and Emergency four hour target. Ambulatory care has not been utilised by primary care colleagues. Audit results were shared with CCG to improve the referral rate by Primary Care. More investment is needed in future in ambulatory care by reinvesting money saved by reduced length of stay.
14. Testicular seminoma in an infertile adult patient with Persistent Mullerian Duct Syndrome.
Shaden Saleh Al Mousa1, Nufe Al Mansor1, Ammar Ashraf1, Mohamed Tahar Yacoubi1, Peter Sylivanus Bahame1, Sohail Iqbal2, Usman Saeed3
1King Abdulaziz Hospital, Ministry of National Guard Health Affairs, Al-Ahsa, Kingdom of Saudi Arabia; 2Wythenshawe Hospital, Manchester University NHS Foundation Trust and 3Royal Blackburn Hospital, UK
Introduction: Persistent Mullerian duct syndrome (PMDS) is an autosomal recessive disorder characterized by the persistence of Mullerian duct derivatives (uterus, cervix, fallopian tubes and proximal vagina) in a phenotypically and karyotypically male patient. This internal male pseudohermaphroditism is usually an incidental diagnosis in children who present with cryptorchidism and inguinal hernia or in adults with cryptorchidism, infertility or an abdominal mass. PMDS is associated with a higher risk of malignant transformation of gonads. Here we present a case of testicular seminoma in an adult infertile patient with persistent MDS. The patient had laparoscopic bilateral orchidectomy with removal of fallopian tubes and commenced on long-term testosterone supplement therapy.
Subjects and Materials: A 42 years old morbidly obese (body mass index 57) infertile male patient had an elective admission for bariatric surgery. During pre-operative assessment, he was investigated for infertility and had an inguinoscrotal ultrasound to locate undescended testes. Postoperatively, he had MRI abdomen and pelvis. Six months later he had an urgent contrast enhanced CT abdomen and pelvis to rule out the causes of his right flank pain.
Results: Pre-operative inguinoscrotal ultrasound revealed no testicular tissue in either the inguinal canals or the scrotum. Genetic screening confirmed 46 XY Karyotyping and hormonal profile showed raised FSH (26.3 IU/L) and LH (14.2 IU/L) and normal testosterone level (11.3 ng/ml). MRI pelvis confirmed the presence of a small, rudimentary uterus and bilateral fallopian tubes and identified bilateral adnexal masses (gonads) measuring about 3 x 2 cm. Emergency contrast enhanced CT abdomen [Figure] showed a complex heterogeneous mass containing some air foci in right iliac fossa with twisted engorged vascular pedicle unrelated to bowel loops, presumed to be a twisted gonad. Following imaging evaluation, patient underwent laparoscopic removal of this mass, mildly congested appendix, normal looking left gonad and both fallopian tubes. Rudimentary uterus was left behind undisturbed. Histopathological analysis confirmed these gonads to be testicles with marked atrophic changes [Figure]. The right-sided testicle showed haemorrhagic infarction consistent with torsion along with a 5.5 cm classic seminoma. Full circumference fallopian tube and fimbria were identified bilaterally. Because of bilateral orchidectomy with normal male karyotype and normal male secondary sexual characters, regular testosterone hormone replacement therapy (testosterone 1000 mg / every 3 month) was instituted.
Conclusion: Patients with persistent Mullerian duct syndrome or internal male pseudohermaphroditism have 46 XY karyotype, near normal development of secondary sexual characters and persistent Mullerian duct structures i.e., uterus, cervix, fallopian tubes and proximal vagina. Our patient was diagnosed very late possibly due to cultural issues and stigmata attached to pseudohermaphroditism.
Figure. Testicular Seminoma – From left to right coronal reconstruction of CT scan and US images depicting RIF mass in red arrow and twisted pedicle in yellow arrow. Histopathology image demonstrate malignant cell proliferation of classical seminomatous non-cohesive, large, round & atypical cells with atypical nuclei owing prominent nucleoli & granular cytoplasm in right gonad.

15. Ovarian germ cell tumours; experience of a regional centre
Douglas Cartwright1, Ashita Waterston2, Jeff White2
1NHS Greater Glasgow and Clyde, 2Beatson West of Scotland Cancer Centre
Introduction Ovarian germ cell tumours are rare but aggressive cancer which have histological and treatment similarities with the more common male germ cell tumours. However the outcomes are poorer for women with germ cell tumours than for men [1]. Historically, in the west of Scotland, female germ cells patients were managed within standard gynaecological cancer services and male patients in a dedicated germ cell unit. Due to the highly specialised nature of the condition and the experience of the clinicians using similar chemotherapy regimens, the management of ovarian germ cells was incorporated into the germ cell unit. We present the experiences of this unit over the last 6 years.
Method We reviewed data from all women with ovarian germ cell tumours treated or followed up under the regional germ cell unit. Fertility is an important consideration for these young women and we investigated the rate of fertility sparing surgery, utilisation of pre-chemotherapy fertility treatments and the rate of successful pregnancies. With the introduction of the Cisplatin, Vincristine, Methotrexate, Bleomycin with alternate Actinomycin, Cyclophosphamide and Etoposide chemotherapy regimen (POMB/ACE) there was a concern that this will cause problems with monitoring during treatment as it associated with elevation of alpha fetoprotein (AFP) levels which is used as a marker or response. We compared AFP levels between POMB/ACE and the bleomycin, etoposide, cisplatin (BEP) regimen used in the adjuvant or neo-adjuvant setting.
Results 26 patients have been treated or followed up by the unit over the last 6 years. Median follow up is 55 months (range 3months – 31 years). The all-cause mortality is 0 and the relapse rate is 19%. Relapses were spread equally through the treatment groups. 21 out of 24 eligible patients received fertility sparing surgery. Of these there has been 6 successful pregnancies following treatment. There was no significant difference in AFP levels between BEP and POMB/ACE groups.
Conclusions Outcomes for ovarian germ cell patients in the west of Scotland are comparable to published case series. The low incidence makes it difficult to identify statistically significant differences however we hope to promote collaboration and gather more data through a national ovarian germ cell database set up through the Scottish Germ Cell Group.
1. Murugaesu N, Schmid P, Dancey G, Agarwal R, Holden L, McNeish I, et al. Malignant Ovarian Germ Cell Tumors: Identification of Novel Prognostic Markers and Long-Term Outcome After Multimodality Treatment. J Clin Oncol. 2006;24:4862–6.
16. A Case of Pyrexia of Unknown Origin and Recurrent Hospital Admissions in a Cardiac Patient
Syed Emir Irfan Wafa¹, Raheel Ahmed², Kay Teck Ling³, Peter Carey³
¹University Hospitals of Leicester NHS Trust, ²University Hospitals of North Midlands NHS Trust, ³University Hospitals Of Derby And Burton NHS Foundation Trust
Introduction Pyrexia of unknown origin (PUO) is defined as a temperature greater than 38.3oC on several occasions, accompanied by three weeks of illness and a failure to reach a diagnosis after one week of inpatient investigations [1]. We describe a case of a 72-year-old man with a significant cardiac history and a pacemaker in-situ presented to the emergency department of a district general hospital with sepsis five days after he had his pacemaker unit batteries changed. He had deranged vital signs, productive cough and pyrexia. He had a normal chest plain radiograph (CXR). However, with right basal crackles on auscultation, he was empirically treated for a lower respiratory tract infection (LRTI) with intravenous antibiotics. The patient was discharged but had to be readmitted four times over the span of 4 months due to recurrent pyrexia. Repeated Trans-thoracic (TTE) and Trans-oesophageal (TOE) echocardiograms, and CT neck/thorax/abdomen/pelvis were done however no evidence of infection was found on the scans. A FDG-PET scan was eventually done which showed evidence of pacemaker-lead infection. His pacemaker unit was removed and replaced with a REVEAL device. He improved clinically with no further hospital admission to date.
Methods Routine blood test only showed raised WCC and CRP. Connective tissue disease screen, viral and tumour markers, syphilis serology, and hepatitis screen were negative. Two out of six blood cultures (on separate admissions) done grew Enterobacter cloacae. Repeated CXRs, CT scans and Echocardiograms showed no evidence of collection/infection. A FDG-PET scan was carried out which detected a focus point of increased activity around the pacemaker leads.
Results Enterobacter cloacae is a nosocomial, gram-negative, facultatively anaerobic, rod-shaped bacterium from the Enterobacteriaceae family. It is usually found in the gut normal flora and skin of humans. It can colonise surgical equipment, operative cleaning solutions and heparin solution used to irrigate certain intravascular devices [2]. The surgical equipment used in this patient’s pacemaker battery change may have been colonised with the bacteria which could explain why it was present in the blood cultures. Another explanation would be that it was a skin commensal for the patient. However, to our knowledge, no other cases from the hospitals involved have been identified or reported recently. Unfortunately, when the pacemaker was removed in our patient, the pacemaker leads were not sent for culture and were discarded. The type of PET scan used in this case was the FDG- PET. Hybrid F18- FDG-PET/CT has high sensitivity and relative non-specificity for malignancy, infection and inflammation [3,4]. The subsequent removal of the pacemaker led to the improvement and resolution of symptoms.
Conclusions This case has highlighted the importance to explore previous hospital admissions, building a timeline of events, which could be leading to the patients’ current presentation. Moreover, patients presenting with pyrexia after a recent prosthetic implantation should be investigated for prosthesis-led-infections, despite negative investigation results. Therefore, the approach to investigate and treat known source of infections and pyrexia of unknown origin needs to be done systematically according to set hospital protocols and evidence-based medicine.
1. Petersdorf RG, Beeson PB; Fever of unexplained origin: report on 100 cases. Medicine (Baltimore). 1961;40:1-30.
2. Mezzatesta ML, Gona F, Stefani S. Enterobacter cloacae complex: clinical impact and emerging antibiotic resistance. Future Microbiol. 2012 Jul;7(7):887-902.
3. Hao R, Yuan L, Kan Y, et al; Diagnostic performance of 18F-FDG PET/CT in patients with fever of unknown origin: a meta-analysis. Nucl Med Commun. 2013;34(7):682-8.
4. Balink H, Verberne HJ, Bennink RJ, et al; A Rationale for the Use of F18-FDG PET/CT in Fever and Inflammation of Unknown Origin. Int J Mol Imaging. 2012;2012:165080. doi: 10.1155/2012/165080.
Figure 1. FDG-PET scan images showing increased focal activity around pacemaker leads.

Figure 2. CT appearances: no evidence of soft tissue abnormality. There is a small focus of increased activity (SUV-max 7) around the pacemaker leads as they pass from the left brachiocephalic vein into the superior vena cava. Increased activity in the right antecubital fossa correlates to some tissuing at the injection site.
17. Establishing a physiologically relevant in vitro model for ischaemic stroke injury in brain endothelial cells Gabriela Warpsinski, Salil Srivastava, Thomas P. Keeley, Paul Fraser, Giovanni E. Mann
King’s College London
Introduction Ischaemic stroke is a major contributor to adult disability in developed countries. However, the only clinically approved acute treatment is delivery of the thrombolytic agent, alteplase, that has a narrow window of 6h post-stroke. To better screen treatments for ischaemic stroke, a more relevant in vitro model for ischaemic stroke is needed. Numerous studies have demonstrated that brain microvascular endothelial cells experience an O2 environment ranging from 4-7 kPa, on the contrary most cell culture studies are conducted under ambient O2 levels, 18 kPa that inevitably expose cells to hyperoxia. To better understand the consequences of O2 levels, mouse brain endothelial cell line, bEnd.3, was cultured long-term under 18 kPa or 5 kPa O2 levels, and cell sensitivity to in vitro model of ischaemic stroke was assessed.
Methods bEnd.3 cells were cultured long term (5 days) under 18 kPa or 5 kPa O2 levels and subjected to oxygen-glucose deprivation (OGD) for 2-12h. Cell viability was then assessed using ethidium bromide staining. Intracellular O2 content was also measured using an O2 sensitive nanoparticle probe, MitoXpress-Intra (2.5 μg/ml), in an O2-regulated plate reader from BMG Labtech. Statistical analysis was performed using student’s t-test or two-way analysis of variance (ANOVA) followed by Bonferroni Post Hoc test.
Results In the present study, the bEnd.3 cell phenotype was determined following long-term (5 days) culture under 18 kPa or 5 kPa O2. Under 5 kPa O2, the intracellular O2 content of bEnd.3 cells was approximately 3.6 kPa O2 (n=3) and this finding is in agreement with other studies that have reported in vivo O2 content of the microvasculature. bEnd.3 cells cultured under 5 kPa also exhibited lower intracellular glutathione content compared to cells cultured under 18 kPa O2 (20.6 vs 29.9 mmol/mg protein, n=4, p=0.003). Furthermore, bEnd.3 cells cultured under 5 kPa O2 exhibited greater sensitivity to OGD-induced cell death, with increased ratio of dead to live cells seen under 2h OGD (0.42 vs 0.05, n=3, p=0.0002).
Conclusions The majority of cell culture studies have conducted experiments under hyperoxia. The present study highlights the importance of conducting cell culture studies under physiological O2 levels, as demonstrated by the different phenotype resulted from long-term culture under physiological O2 levels.
This work was supported by Grant BHF (FS/13/66/30445) from the British Heart Foundation. The authors declare no conflicts of interest.
18. An Assessment of the Smoking Cessation Policy in an NHS Trust
Sachin Ananth,¹ Felicite Mukeshimana,¹ Sanjida Rahman,¹ Nicola Whiteley, ² Louisa Pierce,² Raymond Anakwe²
¹Imperial College School of Medicine, ²Imperial College Healthcare NHS Trust
Introduction Smoking is the second biggest risk factor for premature death in the UK, and it is a significant risk factor for many chronic illnesses. Approximately 25% of secondary care patients smoke, and so treating tobacco dependence would create an opportunity to improve the health of these patients. Referral to stop smoking services is the optimum way to induce smoking cessation- smokers who are referred to these services are four times more likely to quit. NICE guidelines set out the standard of smoking cessation support in secondary care. This audit aimed to assess the compliance of an NHS Trust’s smoking cessation policy with these NICE guidelines.
Subjects and Methods The NICE baseline assessment tool was used to assess the compliance of the Trust’s smoking cessation policy with the NICE guidelines. To evaluate the implementation of the Trust’s policy in clinical practice, snapshot audits of the medical notes of current inpatients and outpatients were undertaken. Medical notes were collected from at least 2 medical specialties and 2 surgical specialties. The notes were assessed for documented smoking status in all patients, and offer of nicotine-replacement therapy (NRT) and referral to a stop smoking service in current smokers.
Results The Trust’s smoking cessation policy was partially compliant with the NICE guidelines; significant gaps in the Trust’s policy included smoking cessation in outpatients and the training of all staff to deliver stop smoking advice. 14/27 (51.9%) of outpatients and 54/80 (67.5%) of inpatients had smoking status documented in their notes. Documentation varied widely across the different specialties, ranging from 0% of Neurology and ENT outpatients, to 100% of Respiratory inpatients. 7/19 (36.8%) of current smokers had a documented offer of NRT, while 4/19 (21.1%) of current smokers had a documented offer of referral to a stop smoking service. Of the 3 current smokers in the Respiratory ward, none were offered NRT and 1 was offered a referral to a stop smoking service.
Conclusions While the Trust’s smoking cessation policy partially complied with the NICE guidelines, implementation of the Trust policy was insufficient. There were low rates of smoking status documentation in many specialties, and so healthcare staff should be encouraged to ask about smoking status, even if it may not seem relevant to the patient’s presenting complaint. Few smokers were offered referral to stop smoking services. Greater awareness of these services is needed, so that smokers receive appropriate smoking cessation support, ensuring that opportunities to improve the health of the nation are not missed.
19. The benefits of an integrated Eye Clinic Liaison officer in improving patient outcomes in Ophthalmology
Mrs Jennifer Bacon – Eye Clinic Liaison officer, Mrs Hayley Coates- Ophthalmic Science Practitioner, Mr Nitin Gupta- Consultant Ophthalmologist
West Suffolk NHS Foundation Trust, UK
Introduction The loss of sight can have a profound impact on a patient’s independence and well-being. Giving patients the devastating news that they are losing their sight is very challenging and when receiving information, a patient often requires considerable support and time. Eye Clinic Liaison officers (ECLOs) are essential in providing patients, their families, and carers with practical and emotional support to help understand their diagnosis. They can help patients not only adapt to living with sight loss, but also to ensure they do not become isolated and retain their independence. ECLOs provide a vital role in bridging the gap between health and social care services, such as fall prevention, job retention, education and social services, enabling early intervention. The service demonstrates how health and social care can work together effectively and this supports the NHS outcomes framework. At the West Suffolk NHS Foundation Trust we have an integrated ECLO. This has proven to reduce DNA’s, reduce clinician time per patient, help patient compliance with treatment, and streamline the process for sight registrations. The Royal college of Ophthalmologists recognised the importance of the role of ECLOs in 2007, in its guidelines to commissioners and clinicians, which recommended the use of ECLO’s as part of Age-Related macular degeneration services.
Methods In order to investigate the aims and objectives, evidence was gathered from Ophthalmologists, Patients and other eye clinic staff, with satisfaction surveys filled by those whom accessed or referred patients to the ECLO service.
Results Surveys were collated and feedback was positive. Having an integrated ECLO has meant timely referrals to appropriate services, providing access to support, and also services such as low visual aids and mental health. Direct access to mental health services reduces the need for GP appointments, meaning that those who require help receive it sooner. Early falls prevention and referrals into the community team have reduced the number of falls for patients with visual impairment, reducing hospital admissions. 95% of surveys received from staff, working with ECLOs, said that it improved the patients experience and reduced time spent in the clinic. Patients felt happier that they were given time to discuss their eye conditions and have access to support. Other staff working within the Eye clinic also felt that they further understood sight loss after receiving visual awareness training. This training was also delivered to other professionals, including occupational therapists, within the hospital who have been better equipped to assist their visual impaired patients.
Conclusions The numbers of patients living with sight loss is gradually increasing the demand on ophthalmic services. Ophthalmic services continue to have the second highest number of outpatient attendances of any speciality, placing enormous pressure on ophthalmic staff to diagnose and treat patients. Having an integrated ECLO at the West Suffolk hospital has proved invaluable. The ECLO service is a good example of how integrated secondary care and social care improve patient outcomes. Evidence has shown that the service is well used and the ECLO service is a vital part of any Eye clinic.
20. Registry report of the prevalence of ECG abnormalities and their relation to patient characteristics in an asymptomatic population.
Adam Ioannou,¹ Nikolaos Papageorgiou,² Donald Singer,³ Constantinos Missouris⁴
¹Royal Free Hospital, ²St. Bartholomew’s Hospital, ³Fellowship of Postgraduate Medicine, ⁴Frimley Health NHS Trust
Background Cardiovascular disease is the leading cause of morbidity and mortality in developed countries. Many patients do not experience symptoms before a first major cardiovascular event. Resting electrocardiogram (ECG) may help identify asymptomatic individuals with a high risk of cardiovascular disease. We sought to determine the prevalence of ECG abnormalities in an apparently symptom-free adult population within a prospective registry.
Methods The registry consisted of 4739 consecutive apparently healthy individuals (age 62.8 ± 6.2(SD) years; 54% female), referred by their General Practitioners between 2009 and 2013. Patient demographics, and clinical data were obtained, alongside blood tests and a resting ECG.
Results ECG abnormalities were present in 1509 (31.8%) subjects and were commoner with increasing age (F=0.161, p=0.01), systolic (F=0.134, p=0.01) and diastolic (F=0.44, p=0.01) blood pressure and waist circumference (F=0.53, p=0.01). Left ventricular hypertrophy (LVH) was the most common abnormality (n=281) and was positively associated with systolic (F=0.12, p=0.01) and diastolic blood pressure (F=0.99, p=0.01), and male gender (X2=60.5, p<0.01). All ECG abnormalities (except for LVH) were associated with an increasing age, while right bundle branch block (F=0.041, p=0.01) and atrial fibrillation (n=29; F=0.036, p=0.05) were associated with the presence of diabetes mellitus (n=211). Only left bundle branch block (n=50) was associated with angina (F=0.05, p=0.01).
Conclusions Unrecognised cardiac abnormalities are common in middle-aged men and women with no overt symptoms. ECG offers the potential to identify these abnormalities and provide earlier intervention and treatment, and possibly improve cardiovascular outcome.
21. Late diagnosis of aberrant origin of right pulmonary artery from ascending aorta and increased morbidity
Sohail Iqbal1, Matthias Schmitt1, Nik Abidin2
1Wythenshawe Hospital/Manchester University NHS Foundation Trust, 2Salford Royal NHS Foundation Trust
Introduction The aberrant origin of a single pulmonary artery is a rare cardiovascular anomaly. So far 131 cases have been reported in English literature. It’s a result of the failure of migration of embryonic branch of a pulmonary artery to reach the pulmonary trunk during embryological period. The aberrant origin of right pulmonary artery from ascending aorta (AORPA) can be associated with patent ductus arteriosus (PDA), atrial septal defect, ventricular septal defect and aortic arch isthmus hypoplasia, whereas, the aberrant left pulmonary artery is associated with the Tetralogy of Fallot. Early and rapid development of pulmonary hypertension is a hallmark of the underlying pathology in untreated cases and the one-year survival is approximately 30% in the absence of any surgical intervention. Hence, early diagnosis and surgical management is mandatory to optimise the outcome.
Subjects and methods We report a case of a 46 years old Caucasian female who presented with progressive breathlessness and productive cough and was investigated to delineate the presence of AORPA and its cardio-pulmonary associations with the help of a follow up CT scan, bronchoscopy and a cardiac MRI (CMR). The patient had a surgical repair of PDA at the age of 3 and remained generally fit and well afterwards however, could never take part in the stamina sports and long distance running due to shortness of breath. In last decade, she had multiple episodes of recurrent respiratory tract infections and intermittent and relapsing allergic bronchopulmonary aspergillosis (ABPA). Her routine bloods showed eosinophilia and the lung function tests demonstrated a restrictive lung disease with FEV1 of 58% and vital capacity of 69% (predicted). She also had an asthma quality life questionnaire that scored 5.3. She had a HRCT chest seven years ago that showed right middle and lower lobe changes in line with the diagnosis of ABPA, AORPA with the signs of pulmonary hypertension, a slit like compression of the right main bronchus and the right pulmonary arterial wall focal calcification. She had not had any surgical intervention for AORPA and her symptoms got worse overtime.
Results Both follow up CT chest and bronchoscopy revealed mechanical compression of the right main bronchus and extensive mucous plugging [Figure]. CT chest demonstrated interval progression with the development of a new large area of consolidation in right middle and lower lobes, right perihilar bronchiectasis and reactive mediastinal lymph nodes. CMR confirmed the anomalous origin of the right pulmonary artery from the posterior aspect of the ascending aorta and displayed the features of right lung hyperaemia [Figure]. The right pulmonary artery, aortic root and the ascending aorta were dilated.
Conclusion Anomalous right pulmonary artery is usually diagnosed in early childhood, but our patient was diagnosed in adult life possibly due to the early surgical treatment of PDA that might have delayed the clinical presentation. The delayed diagnosis increased her morbidity and affected the quality of life; therefore, we recommend early investigation and surgical management planning.
Figure. First row from left to right CXR – prominent hilar vessels; CT lung window – Infective changes; CT mediastinal window – Abnormal origin of right pulmonary artery from aorta with calcification; Cardiac MRI T1 image – dilated aorta and AORPA. Second Row from left to right 3D and MIP reformatting – showing this anomaly with right sided pulmonary hyperaemia; Bronchoscopy images – mucous secretions and bronchomalacia

22. An Audit of Adult VTE Risk Assessment Compliance with NICE Guidelines
Sanjida Rahman¹, Sachin Ananth¹, Felicite Mukeshimana¹, Nicola Whiteley², Raymond Anakwe²
¹Imperial College School of Medicine, ²Imperial College Healthcare NHS Trust
Introduction Venous Thromboembolisms (VTEs) are often preventable. In the UK, 60% of all VTEs are hospital-associated, costing the NHS approximately £200 million. VTE risk assessments ensure patient safety and reduce the economic healthcare burden of complications. According to NICE guidelines (NG89), risk assessments should be performed on all patients on admission, however, the NHS Quarter 4 2017/18 assessment showed 1992 inpatients were not VTE risk assessed at Imperial College NHS Trust (ICHT) between January to March 2018. This audit aimed to better understand the strengths and weaknesses of ICHT’s performance to allow clinical leads and risk owners to formulate an action plan to close these gaps.
Subjects and Methods The ICHT Adult VTE Trust policy was assessed using the relevant baseline assessment tool for NICE guidelines NG89. Seven quality statements corresponding to NICE Quality Standard 3 (QS3) and the Trust policy were used to develop the audit tool for assessing the Trust’s performance. At St Mary’s Hospital, 60 consecutive inpatients, across 6 different specialties, formed the sample population. Data was collected between 6th August until 13th August 2018 using ICHT electronic health record, CERNER. Analysis of the data applied ICHT Trust’s Assurance rating for each sub-finding. Ethical principles and procedures adhered to standards set by the World Medical Association (WMA) Declaration of Helsinki and ICHT.
Results Eight of the total 60 patients, did not have accessible VTE risk assessment forms, either due to blank forms submitted (2/8) or no form being submitted (6/8). The mean time to initial assessment was 38.6 hours. There were four patients whose initial VTE assessments were documented more than 6 days after inpatient admission; 3 out of 4 of these exceeded 16 days post-admission. The audit results showed that compliance rate of initial assessment and reassessment is currently below target at 91.7% and 78.2% respectively. Thirty-seven patients were at risk of thrombosis and had no contraindications to thromboembolism-deterrent stockings (TEDS). Despite this, 21 out of 37 of these patients were not prescribed TEDS. Forty two patients were prescribed pharmacological prophylaxis, however only 20 out of 42 had been weighed prior to prescription. A 0% compliance rate was found regarding documentation that high-risk patients received written VTE prevention information on admission.
Conclusions The main areas of improvement identified were to ensure VTE assessment and reassessment were completed for all inpatients and to reduce the mean time to initial assessment. Patient education should also be improved by providing written VTE prevention given to high-risk patients on admission and in pre-operative assessment, ensuring this is documented on CERNER. Mechanical prophylaxis (TEDs) should be appropriately prescribed to non-contraindicated patients at risk of thrombosis. In addition, the weighing of all patients prior to the prescription of pharmacological VTE prophylaxis also requires improvement to ensure the correct dose is given. A larger trust-wide audit is needed to consolidate these findings and follow patients to discharge to determine compliance to Statements 6 and 7 in NICE QS3.


